
Cogdog (CC), Flickr
Happy New Year, constant readers. There’s no question that the big public health story of 2014 was Ebola. The African epidemic has now racked up more than 20,000 cases, according to the World Health Organization, which has put together a useful map and timeline of developments since March. If you’d like to look back on the year, the best sum-up by far is the New York Times’ long and beautifully told “How Ebola Roared Back,” and for a sense of what we learned this year — and what we still don’t know — consider reading Helen Branswell’s account, published at the Winnipeg Free Press.
The international health community still must focus on Ebola; the disease is by no means contained. But my New Year’s wish, for those of us outside that community, is that we begin 2015 by accepting that wherever diseases occur, they are going to travel. We had repeated demonstrations of this with Ebola; and as a global community, we didn’t react well. (If you feel like revisiting the cringe-making details, the Today in Ebolanoia Tumblr is still up.)
The disease that really makes this case, though, is the antibiotic resistance factor NDM. Since its original discovery in one person in Sweden in 2008, this snippet of DNA — which makes common infections essentially untreatable — has been carried by patients to at least 40 countries, and spread within those countries to create local hospital outbreaks.
That’s a lot of border-crossing.
To recap: NDM (New Delhi metallo-beta lactamase, named for its city of presumed origin) is a gene, which directs production of an enzyme, which arms bacteria to protect themselves against almost all of the hundreds of antibiotics available to medicine. The gene tends to be found in bacteria that are carried in the gut and that leak out, and contaminate the environment, during treatment in an intensive care unit: E. coli, Klebsiella, Acinetobacter, and a few others. For some patients infected with bacteria carrying NDM, two drugs — both of them imperfect and with side effects — have been effective; in some cases, one drug; in some cases, none. Those patients died of untreatable infections. (Past posts on NDM — originally called NDM-1 — are here.)
Because those bacteria live benignly in the gut most of the time, that someone is carrying the resistance factor is invisible to any test or screening regimen; thus, as you can imagine, it walks and flies easily across international borders. Here’s a map from a paper published in 2013 of how far this resistance factor has spread from its first identification in Sweden and its presumed home in India.
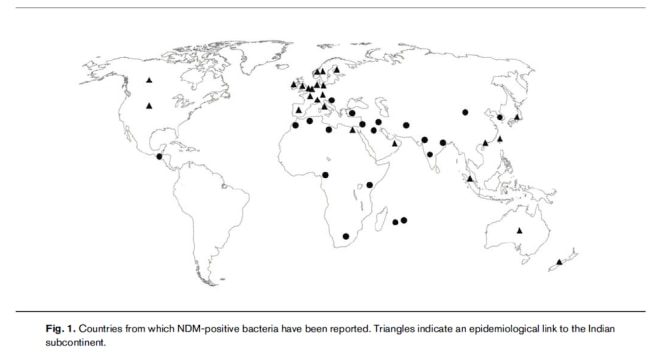
From Johnson and Woodford, 2013. Original here.
Bacteria carrying NDM spread easily in hospital rooms, on equipment, and on the hands of healthcare personnel — so when NDM lands in a new country, it frequently causes local outbreaks. (As it did in a Denver hospital in 2012.) There is no routine surveillance for the presence of NDM, so it is hard to derive a case count. But when a team who were using Google Maps to trace outbreaks counted up at the end of 2012, they found that almost 800 cases had occurred in four years, all over the globe.
You’ll notice that, unlike Ebola, there hasn’t been any NDM-oia. In fact, outside of the medical literature, there has been remarkably little discussion of the threat. (Outside of this blog, I wrote about NDM for Scientific American in 2011 and Nature in 2013, and Jason Gale at Bloomberg has covered the problem consistently. The New York Times reported on it in early December, wrapping up several years’ worth of news.)
Here’s the point: The under-reaction to NDM and similar globe-spanning resistance threats is as misguided as the over-reaction to the global movement of Ebola was. Neither deals with the threat appropriately. In 2015, we could a do better job protecting public health, as well as spending scarce public funds, if we stayed alert to border-crossing diseases and gave them the attention they deserve.
Cites:
- Berrazeg M, Diene SM, Medjahed L, et al. New Delhi Metallo-beta-lactamase around the world: An eReview using Google Maps. Euro Surveill. 2014;19(20):pii=20809.
- Johnson AP and Woodford N. Global spread of antibiotic resistance: the example of New Delhi metallo-β-lactamase (NDM)-mediated carbapenem resistance. J Med Microbiol April 2013 vol. 62 no. Pt 4 499-513.