
Image: AnotherPintPlease (CC), Flickr
The Centers for Disease Control and Prevention today released their annual survey of foodborne illnesses in the United States, and the news is, well, not great. In the words of the press announcement they sent out to announce the data release: “limited progress.”
The survey — technically the Foodborne Diseases Active Surveillance Network, but usually known as FoodNet — doesn’t cover the entire US; it’s a representative sample drawn from 10 sites in nine states where the CDC already has arrangements with epidemiologists and laboratory personnel. Those 10 sites, most of them at state health departments, cover 48 million people, or about 15 percent of the US population. So among that slice, in 2013, there were:
- 19,056 lab-confirmed foodborne illnesses,
- 4,200 of which were severe enough to cause the person to be hospitalized,
- and 80 of which caused the person’s death.
(For context, the CDC’s extrapolation of foodborne illness nationwide, made in 2011, was 48 million illnesses, 128,000 hospitalizations and 3,000 deaths.)
The agency compared the 2013 numbers against two sets of data, one set taken covering 2010-12 and the other 2006-08. Its summation, from its report in its weekly publication MMWR:
Compared with 2010–2012, the estimated incidence of infection in 2013 was lower for Salmonella, higher for Vibrio, and unchanged overall. Since 2006–2008, the overall incidence has not changed significantly. More needs to be done.
Here’s a handy cheat sheet for the major fooodborne organisms, distributed by the CDC. Note that none of the smileys are actually smiling:
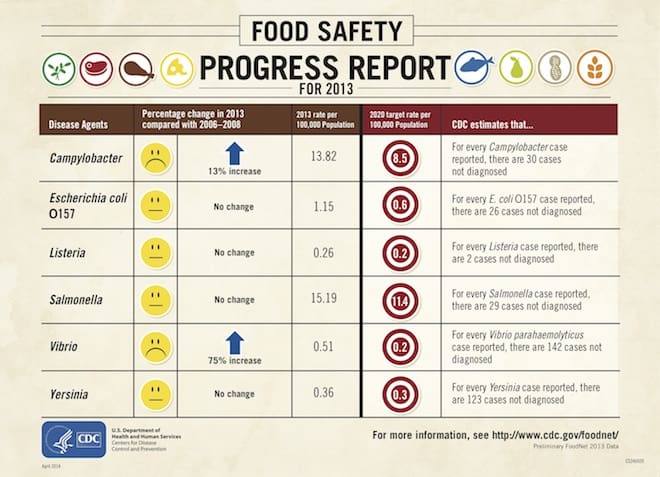
Image courtesy CDC.gov; original here.
That graphic is a little misleading in that it lists the problem organisms alphabetically. Of the six organisms, Salmonella causes the most illness, at 38 percent of the reported infections; Campylobacter comes second, at 35 percent. Vibrio, which had the largest increase, causes only 1 percent of infections.
If you know anything about bad bugs and food, those first two may sound familiar; they’re often associated with chicken, the meat that we in the United States eat the most of. (Vibrio is most associated with shellfish.) Why would two chicken-related organisms be problematic? The CDC report provides a clue: There is no federal standard for how much Campylobacter can be present on chicken, and the federal standard for the presence of Salmonella has not kept up with changes in what chicken Americans buy. From the MMWR:
In 2011, USDA-FSIS tightened its performance standard for Salmonella contamination of whole broiler chickens; in 2013, 3.9% of samples tested positive. Because most chicken is purchased as cut-up parts, USDA-FSIS conducted a nationwide survey of raw chicken parts in 2012 and calculated an estimated 24% prevalence of Salmonella.
Tightening standards for whole birds when people buy cut-up ones sounds like a chicken version of looking under the streetlamp for the keys you dropped, because the light is better there. But to be fair: The USDA apparently noticed this mismatch and, last year, proposed a Salmonella action plan, including an examination of contamination issues for chicken parts, and also is working on new Campylobacter standards. (I’ll try to do more on this after the holiday.)
The needle didn’t budge either for E. coli infections from the severe, toxin-producing strain O157:H7, which causes a kidney-overload syndrome that can kill young children. (If you’ve been reading for a while, you might remember that O157:H7 has been considered a zero-tolerance “adulterant” in food since 1994, but other similar “STECs” — toxin-producing E. coli strains — only got that regulatory status in 2011.) . Reacting to the numbers, the Consumer Federation of America said in a statement:
Progress on reducing illnesses from E. coli O157:H7 looks to have stalled and in fact, may be trending back upwards after several years of success. Also troubling is that illnesses from non-O157:H7 STECs continue to trend upwards. Illnesses from E. coli O157:H7 and non-O157 STECs have shown no significant change when compared to the 2006-2008 baseline. In addition, for the third year in a row, the incidence of illnesses from non-O157 STECs is higher than illnesses from E. coli O157:H7.
Finally, a troubling issue emerged during the CDC’s press briefing, mentioned by Dr. Rob Tauxe, deputy director of the agency’s foodborne-illness division. To get diagnoses made more quickly — and thus get patients medical help faster — public health labs have begun using rapid tests that recognize a molecular signature, instead of the traditional culture-based tests that grow the bacterium on a dish and test it. This has a significant downside: No organism means no ability to do the “DNA fingerprinting” that the public health system relies on for PulseNet, a crucial tool that can link infections that occur many miles away from each other. Reacting to that, Caroline Smith DeWaal of the Center for Science in the Public Interest said in a statement:
It is critically important that CDC develop a plan to address the increasing use of diagnostic tests that don’t use lab cultures. Otherwise the trend of declining reporting of outbreaks may continue—not because fewer people are getting sick, but because state health departments and CDC cannot track the outbreaks.
I’ll add one thing to that. Not having a cultured organism also means losing the ability to detect when the foodborne illness is antibiotic-resistant, because resistance assays at the moment rely on having living bacteria. Antibiotic resistance is an increasingly important issue for food production; the now year-long outbreak in chicken from Foster Farms, which has racked up 524 infections in 25 states, involves a Salmonella that is multi-drug resistant. No longer being able to track resistance could mean completely losing track of foodborne epidemics.
We know this can happen, because it already did happen, for gonorrhea, which currently is veering toward untreatability all over the world. As I reported two years ago at Scientific American and here, multi-drug resistant gonorrhea got out ahead of us because public health’s switch to inexpensive rapid tests for STDs sacrificed the ability to examine whether the bacterium’s resistance profile was getting worse. For that to happen to foodborne illnesses as well would be a backward step for public health.